In South Sudan, the Health Pooled Fund 3 (HPF3) consortium, led by Crown Agents and supported by the UK Foreign, Commonwealth and Development Office (FCDO), the European Union (EU), the United States Agency for International Development (USAID), Canada, GAVI and the Swedish International Development Cooperation Agency (SIDA), operates in one of the most challenging contexts, and with some of the worst health indicators in the world. There are often concurrent emergencies to address, such as extreme food insecurity, locust plagues, disease outbreaks and displaced populations resulting from civil or political instability. Despite recent positive developments on the political front, including a government of national unity, South Sudan has also been facing an escalation of inter-communal violence. The recent outbreak of COVID-19 has only exacerbated an already difficult situation in the country.
The first case of COVID-19 was announced in South Sudan on 5th April 2020. Since then, the government has imposed measures to curb the spread and respond to competing health needs for communities, particularly with a focus on women and children. The measures restricted travel among the states as well as a dawn to dusk curfew. Additionally, restrictions were introduced on the number of persons allowed on vehicles and boba bodas (public motorcycles). This new reality imposed on communities had mixed reactions from citizens, which resulted in various challenges, such as health rumours, misinformation and stigma.
HPF’s response and strategies
As a key partner supporting South Sudan’s health care system, the HPF Programme recognises the urgency for the Ministry of Health to respond to the COVID-19 pandemic. The pandemic poses a considerable threat to vulnerable populations and may negatively impact health gains achieved in the country since the civil war. At Crown Agents, we are determined to ensure that basic health services remain accessible to the most vulnerable despite the threat of COVID-19. We do so by strengthening local capacity and delivery, and our HPF programme is at the forefront of these efforts. With restrictions to movements between states, the HPF team has revised activities to apply new, innovative ways of ensuring that the programme’s implementing partners can deliver essential health services to 80% of South Sudan without compromising on quality. Thus, the programme has succeeded in continuing to pursue its core objectives.
COVID-19 preparedness and initial response
At the onset of the pandemic, the HPF team verified onsite how prepared programme partners were for COVID-19 and supported them in developing their readiness and response plans. We also started to sensitize South Sudanese communities to the risks of COVID-19 in HPF supported health facilities and clinics.
Distribution of essential medical supplies
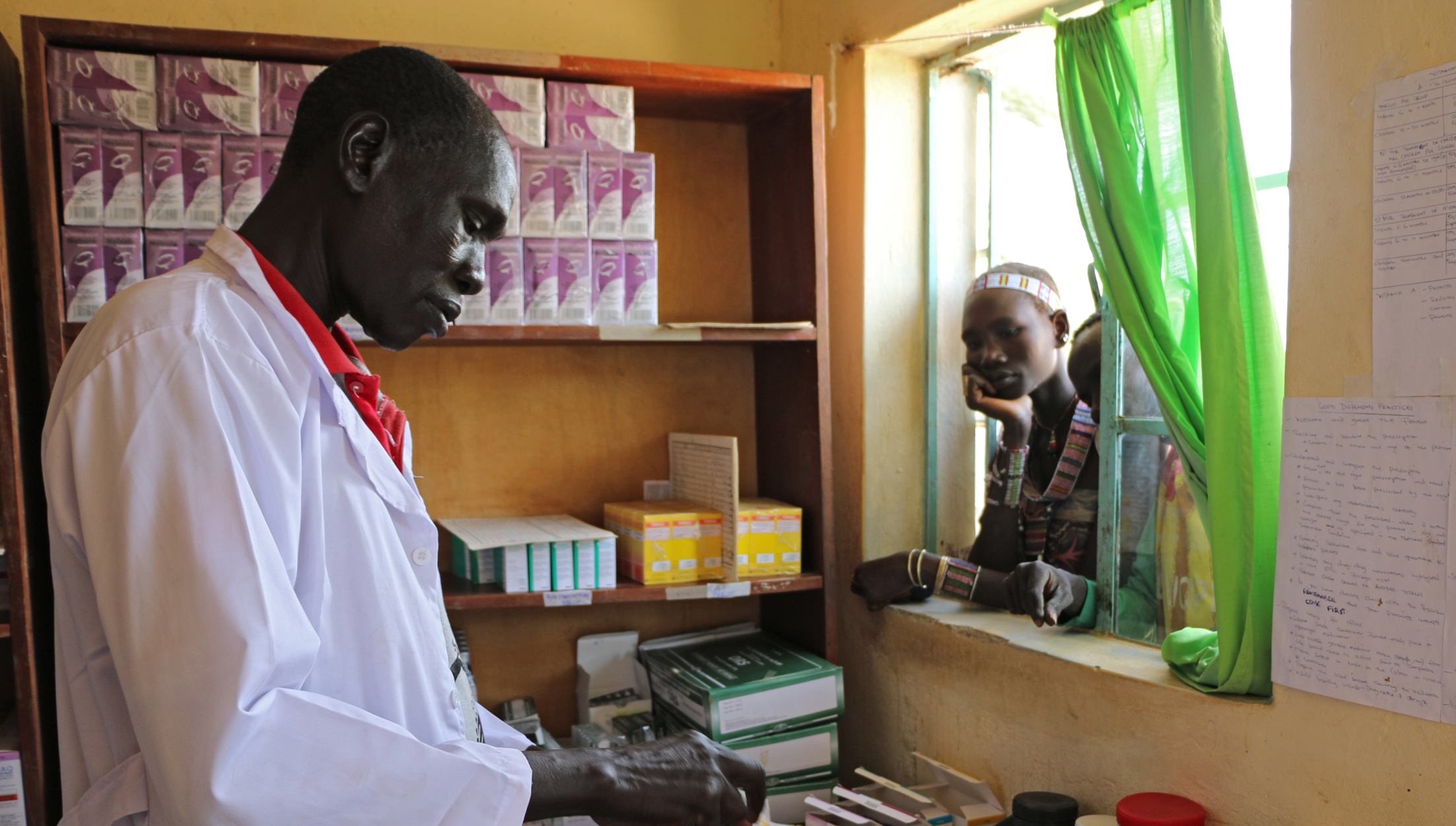
 One of the major challenges that South Sudan has had to address was- and still is- ensuring that commodities and medical equipment reach facilities and communities who need them most. With the HPF programme having a prominent supply chain role in the region, the programme made significant efforts to procure and facilitate distribution: Initially, we distributed a first consignment of PPE donated by World Food Programme (PPE) in Juba, South Sudan. However, as it became obvious that the virus was continuing to spread across the world, the programme ramped up its response. By May 2020, the HPF team was preparing to deliver over 400 tonnes of medicines and PPE kits to the eight states. The significance of these distributions was highlighted by the fact that they were flagged off by the Minister of Health in South Sudan, Hon. Elizabeth Achuei. These shipments did not come without their challenges – there were delays at the border due to COVID-19 testing and clearances, as well as safeguarding concerns, however these were all navigated successfully by the team on the ground.
One of the major challenges that South Sudan has had to address was- and still is- ensuring that commodities and medical equipment reach facilities and communities who need them most. With the HPF programme having a prominent supply chain role in the region, the programme made significant efforts to procure and facilitate distribution: Initially, we distributed a first consignment of PPE donated by World Food Programme (PPE) in Juba, South Sudan. However, as it became obvious that the virus was continuing to spread across the world, the programme ramped up its response. By May 2020, the HPF team was preparing to deliver over 400 tonnes of medicines and PPE kits to the eight states. The significance of these distributions was highlighted by the fact that they were flagged off by the Minister of Health in South Sudan, Hon. Elizabeth Achuei. These shipments did not come without their challenges – there were delays at the border due to COVID-19 testing and clearances, as well as safeguarding concerns, however these were all navigated successfully by the team on the ground.
Ongoing community engagement and development of Information, Education and Communication (IEC) materials
 We also ensured that risk and behaviour change communication was treated as a priority in order to raise awareness within the communities. As Boma health workers[1] were already engaged in the programme and present in their communities, the programme took the opportunity to upskill these workers, enabling them to pass on correct and consistent information on the virus and the risk of infection within their communities.
We also ensured that risk and behaviour change communication was treated as a priority in order to raise awareness within the communities. As Boma health workers[1] were already engaged in the programme and present in their communities, the programme took the opportunity to upskill these workers, enabling them to pass on correct and consistent information on the virus and the risk of infection within their communities.
To spread risk communications as widely as possible, the HPF team has continued to engage with Eye Radio FM, which has an estimated audience of 10 million. Using their weekly slot, HPF experts are addressing rumours, misinformation and disinformation relating to COVID-19. The public also has an opportunity to call in and engage with the specialists asking both pandemic and health related questions, understanding the danger other illnesses still pose to the population.
To address the need for context specific and easy to understand information, we continue to formulate, design, print and distribute IEC material in South Sudan. By the end of June 2020, over 25,000 IEC materials, including COVID-19 risk communication posters, referral pathways to the Ministry of Health and job aids on home management of COVID-19-like symptoms were translated and distributed.
Future programming
With the steady rise in COVID-19 cases, the need for PPE is more critical than it has ever been in South Sudan. Crown Agents is responding to this need, with more consignments due to be distributed across the country in the coming months. Additionally, the HPF team will continue working with the Ministry of Health to ensure that risk communication translates to behaviour change within communities in South Sudan. With no proven vaccine or medicine available, the HPF team, through its implementing partners, is working around the clock to ensure no lives are lost due to avoidable circumstances and treatable conditions.
[1] A community member(s) selected by the members of a Boma to provide community health services to the community (BHW). The BHWs are trained on how to treat and diagnose uncomplicated malaria, diarrhoea and pneumonia and refer severe cases to the nearest health facility.