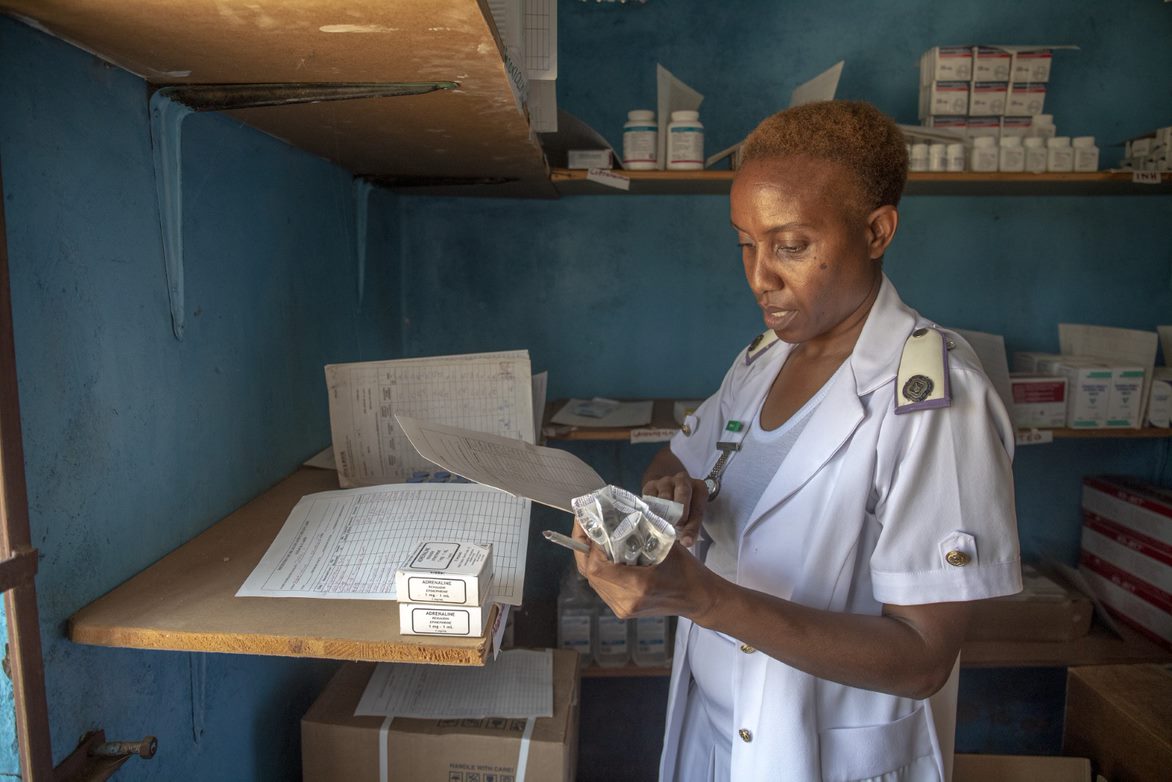
Book an appointment, see a General Practitioner, get referred, wait for the letter, see the specialist.
Many medical systems in the developed world refer thousands of patients to healthcare specialists without complications or cost. Yet, for some getting to see a health expert is a struggle, and for those with limited funds, the process can be near impossible.
In Zimbabwe, great strides have been made to ensure that the most vulnerable are able to receive quality healthcare and can be treated by professionals, even if they can’t afford the necessary costs.
A significant contribution to the effort has come from local level decision-making, fuelled by health facility staff across the country. These staff are part of the Results-Based Financing Programme in Zimbabwe which is managed by Crown Agents and works in partnership with the Ministry of Health and Child Care.
 Through this programme, health service providers are given financial resources as an incentive based on the results they obtain, encouraging the staff to strive for performance targets. The staff are also empowered to make decisions on how best to invest the clinic’s earnings to improve services. The result has been local level decision-making that responds to the specific needs of the local population and sets a constant cycle of enhancement and improvement in healthcare services, particularly in rural areas.
Through this programme, health service providers are given financial resources as an incentive based on the results they obtain, encouraging the staff to strive for performance targets. The staff are also empowered to make decisions on how best to invest the clinic’s earnings to improve services. The result has been local level decision-making that responds to the specific needs of the local population and sets a constant cycle of enhancement and improvement in healthcare services, particularly in rural areas.
In the Mutasa District, healthcare staff under the programme pioneered a new referral system which linked the more rural district clinics with larger hospitals in the area. Patients in rural areas are assessed by the clinic and where necessary referred to the hospital which is equipped with highly trained doctors and medical equipment.
For Bridget Phiri, a local woman living with a disability, this referral system likely saved both her and her child’s life. Bridgit was considered at high-risk for delivering her baby should they attempt a natural delivery at the clinic. Committed to ensuring Bridget’s safety, the Sister-in-Charge (SIC) of her antenatal care unit, Betty Makuwaza, made it her priority to escalate the case.
Betty engaged the Health Centre Committee (HCC) to arrange for an emergency referral to Hauna District Hospital. “We do not have a caesarean section at our clinic. [Bridget] needed access to adequate equipment and well-trained specialists should challenges with her birth occur.”
The distance to the hospital, in this case 20km, would have deterred many women from choosing to give birth there. Some would have instead opted for dangerous home births, where skilled workers are not present to support should complications, such as post-partum haemorrhage, occur. This is a huge contributing factor to high mortality rates in Zimbabwe, which currently stand at 462 mothers out of 100,000 live births.
Expenditure also plays a role: Although the RBF programme is working towards the abolishment of user feeds, patient transportation and caesarean sections can cost patients upwards of $300. For Bridget, her disability made finding work difficult and with a monthly income of $20, the costs were higher than she could afford.
Yet, under the new referral system, the clinic was able to put funds towards Betty’s transportation and operation.
“If it had not been for the compassion of Betty Makuwaza and RBF’s effective referral system, there is a possibility that myself, my baby or both of us could have died. I hope this programme will go a long way in ensuring quality, safe deliveries – especially for those who are disabled.” Bridget said following the safe birth of her baby girl.
Recently, the Results-Based Financing Programme, which is funded through a collaboration between development partners and the Government of Zimbabwe treasury, has been the focus of a study conducted by an independent consultant to assess its value for money as a programme. Results from the study showed the Crown Agents-led RBF approach in Zimbabwe to be extremely cost-effective, reducing operating costs by 59% over 5 years.
 By delivering the programme in a cost-effective manner, more resources have been freed up for the Ministry of Health and Child Care, Zimbabwe and health facilities across the country to spend on healthcare initiatives, such as the referral scheme, to improve the system long-term across the country.
By delivering the programme in a cost-effective manner, more resources have been freed up for the Ministry of Health and Child Care, Zimbabwe and health facilities across the country to spend on healthcare initiatives, such as the referral scheme, to improve the system long-term across the country.
Yet, it is stories like Bridget’s that bring to life the programme’s real value for money. By encouraging staff to pioneer health initiatives such as the referral system, and by efficiently managing funds for the greatest impact, Bridget was able to safely bring new life into the world – something that for her meant more than ‘its weight in gold’!